- Find Us At - Innovation Central, 10 John Williams Blvd South, Darlington, DL1 1BF
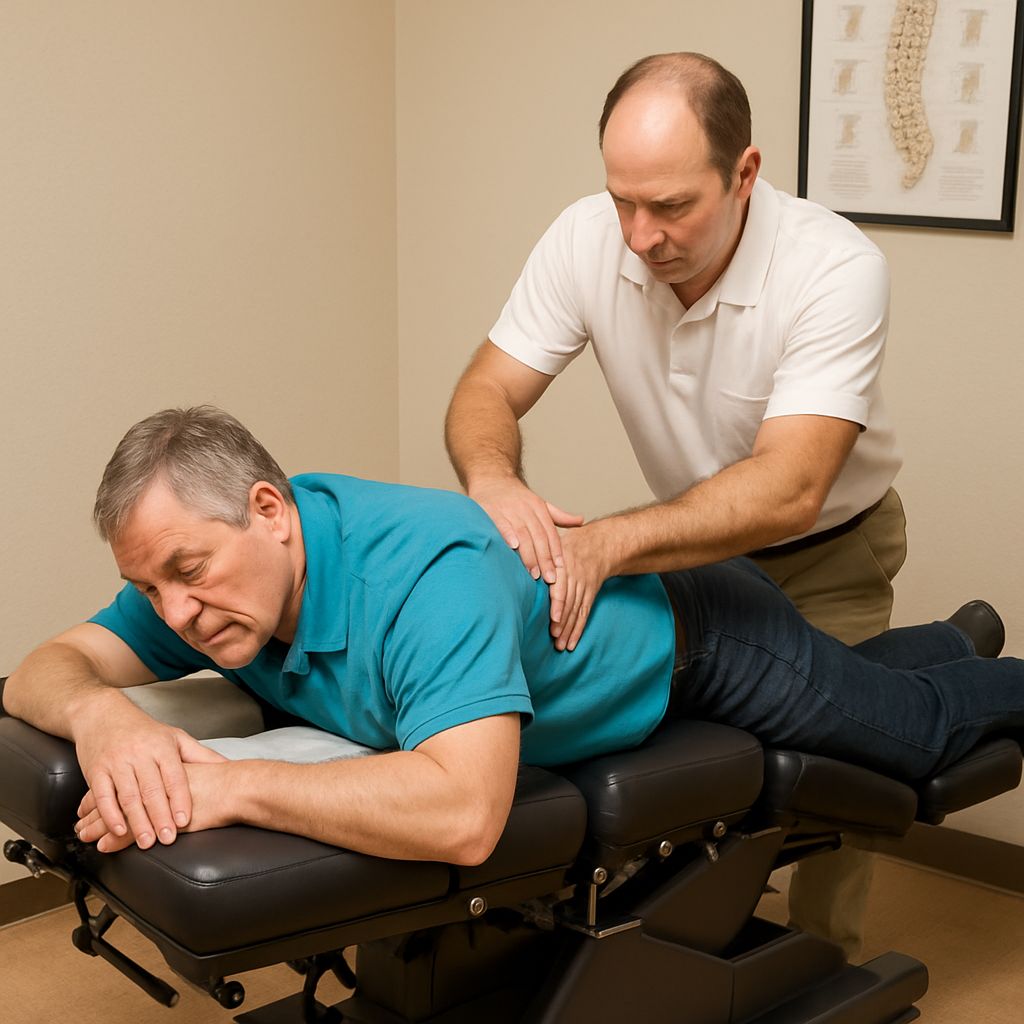
Most people diagnosed with spinal stenosis are handed a prescription or a referral to a surgeon — but there is a third path that millions are taking first.
Chiropractic care has emerged as one of the most sought-after non-invasive treatments for spinal stenosis. In fact, a large multicenter observational cohort study conducted as part of the SPORT study found that 33% of 368 subjects diagnosed with spinal stenosis had already sought chiropractic treatment. That is not a small number. It reflects a growing understanding that the spine can be treated mechanically, without cutting or medication, and still produce real, measurable relief.
For those navigating this condition, resources like chiropractic spinal stenosis relief guides can help bridge the gap between diagnosis and action, explaining what to expect from treatment before ever stepping into a clinic.
The core principle behind chiropractic treatment for spinal stenosis is straightforward: if narrowed spinal spaces are compressing nerves and causing pain, targeted manual therapies can reduce that compression, restore alignment, and give the nervous system room to function properly again. The body often does the rest.
Spinal stenosis occurs when one or more of the bony openings within the spine begin to narrow, reducing the available space for nerves to pass through. This narrowing can happen in the spinal canal itself — called central stenosis — or in the smaller openings where nerve roots exit the spine, called foraminal stenosis. The lumbar spine, or lower back, is the most commonly affected region, though cervical stenosis in the neck is also widespread.
The result is nerve compression. Compressed nerves produce a recognizable cluster of symptoms: radiating pain down the legs, numbness, tingling, muscle weakness, and a characteristic cramping that appears after walking short distances and fades when sitting or leaning forward. This last symptom, called neurogenic claudication, is one of the hallmark signs of lumbar spinal stenosis.
The spinal canal is not a rigid, fixed tunnel — it changes shape slightly depending on your posture. When you extend your spine backward, the canal narrows. When you flex forward, it opens. This is why people with spinal stenosis instinctively hunch forward when walking, and why pushing a grocery cart often provides temporary relief. The body is making its own mechanical adjustments, even without knowing the anatomy behind it.
What causes the narrowing in the first place? The most common culprit is degenerative change — the gradual breakdown of spinal structures over time. Bone spurs form on vertebrae, intervertebral discs lose height and bulge outward, ligaments thicken and become less pliable, and facet joints enlarge. Any one of these changes can eat into the already limited space inside the spinal canal. When multiple changes occur together, the compression becomes significant.
Age is the primary risk factor. Spinal stenosis is most commonly diagnosed in adults over 50, though younger individuals with congenital spinal abnormalities or prior spinal injuries can develop it earlier. The condition does not appear overnight — it develops slowly, often silently, until nerve compression reaches a threshold where symptoms become impossible to ignore.
Left unaddressed, the degenerative changes driving spinal stenosis do not stabilise on their own. Bone spurs continue to grow, disc height continues to decline, and postural compensation patterns — the unconscious ways your body tries to offload pain — start creating secondary problems in the hips, knees, and shoulders. The original stenosis becomes surrounded by a cascade of musculoskeletal dysfunction.
Reduced mobility compounds the problem further. When pain limits movement, the muscles supporting the spine weaken from disuse. Weaker muscles place more mechanical load on already compromised spinal structures, accelerating the very degeneration causing the symptoms. It is a cycle that, without intervention, trends in one direction only.
Chiropractic care approaches spinal stenosis from a mechanical standpoint — identifying where the spine is misaligned, where movement is restricted, and where nerve compression is occurring, then applying precise, targeted techniques to address each issue directly.
Spinal manipulation is the foundational technique in chiropractic care and involves applying a controlled, sudden force to specific vertebral joints to restore proper alignment and movement. For spinal stenosis, this is used carefully to reposition spinal segments that may be contributing to canal narrowing or nerve root irritation.
The goal is not to force a dramatic correction but to gradually restore normal joint mechanics. When vertebrae are properly aligned, disc pressure normalises, ligament tension decreases, and the available space within the spinal canal can functionally improve. Many patients report a reduction in radiating leg pain and local back stiffness following a series of manipulations — not after the first session, but progressively over several weeks of consistent care.
The flexion-distraction technique is one of the most specifically suited chiropractic methods for lumbar spinal stenosis. Developed by Dr James Cox, this gentle, non-thrusting procedure uses a specially designed table that allows the chiropractor to flex, distract, and decompress the lumbar spine in a slow, rhythmic motion.
Unlike high-velocity spinal manipulation, flexion-distraction does not involve a rapid thrust. Instead, the chiropractor manually guides the spine through a range of flexion movements while the lower half of the table drops away, creating a gentle traction effect. This opens the posterior disc space, reduces intradiscal pressure, and widens the spinal canal — directly addressing the structural changes causing stenosis symptoms.
Clinical application of this technique typically involves positioning the patient prone on the Cox table, securing the pelvis, and applying a series of gentle, repetitive flexion movements to individual lumbar segments. The average session using this technique lasts approximately 15 to 20 minutes, and patients generally tolerate it well, including those who have found other manual therapies too painful.
Chronic poor posture is both a consequence of spinal stenosis and a contributor to it. The instinctive forward lean many stenosis patients adopt provides temporary nerve relief, but over time, it places enormous strain on the lumbar discs, thoracic spine, and cervical region. Chiropractors evaluate posture as part of a comprehensive stenosis assessment and develop correction strategies that address these compensatory patterns.
Postural correction in a chiropractic context involves more than reminders to “stand up straight.” It includes identifying muscle imbalances that pull the spine out of alignment, mobilising restricted joints that prevent neutral posture, and training the neuromuscular system to maintain corrected positions during daily activity. For stenosis patients, even small postural improvements can meaningfully reduce the mechanical load on compressed spinal segments throughout the day.
Spinal decompression therapy takes the mechanical principles behind flexion-distraction and scales them up using a motorized traction table that delivers precise, computer-controlled distraction forces to the spine. For spinal stenosis specifically, it is one of the most direct non-surgical methods available for creating meaningful space within a compressed spinal canal.
The therapy works by intermittently stretching and relaxing the spine in a controlled pattern. This alternating cycle creates a negative intradiscal pressure — essentially a vacuum effect inside the disc — that can retract bulging disc material and encourage the flow of nutrients, oxygen, and hydration back into degenerated discs. For stenosis patients, the cumulative effect of repeated sessions is a gradual reduction in the structural crowding that is compressing spinal nerves. Learn more about spinal stenosis treatment.
The traction table used in spinal decompression therapy is a split-design table with a fixed upper section and a lower section that slides in response to computer-controlled tension. The patient lies face down or face up, depending on which spinal region is being treated, and a pelvic harness is secured around the hips and lower torso. A separate thoracic anchor stabilises the upper body.
The computer then delivers a series of distraction cycles — pulling the lower section of the table away from the upper section at a precise angle, holding the stretch for a set duration, and then releasing tension gradually. The angle of distraction can be adjusted to target specific spinal levels. For lumbar stenosis at L4-L5, for example, the table angle is calibrated to focus decompression force directly at that segment rather than distributing it across the entire lumbar spine.
Distraction forces typically range from 50% to 100% of the patient’s body weight and are built up progressively across the first several sessions. A full course of spinal decompression for spinal stenosis usually involves 12 to 20 sessions delivered over four to six weeks, with each session lasting approximately 30 to 45 minutes, including setup time.
Most patients describe the sensation during spinal decompression as a gentle, rhythmic stretching — not painful, but distinctly felt. Some report immediate relief of leg symptoms during the session as nerve pressure is temporarily released. Others notice improvement in the hours following treatment rather than on the table itself. Both responses are considered normal and clinically relevant. For more information on spinal stenosis and how chiropractic care can help, visit this comprehensive guide.
It is common for chiropractors to combine spinal decompression with adjunct therapies during the same appointment. Cold laser therapy, electrical muscle stimulation, or moist heat applied to the lumbar region immediately before or after decompression can enhance tissue response and reduce post-session muscle soreness. Patients are typically advised to avoid strenuous physical activity on treatment days and to stay well hydrated to support disc rehydration between sessions.
Chiropractic adjustments and decompression therapy address the structural side of spinal stenosis, but the muscular system surrounding the spine plays an equally critical role in long-term relief. Without adequate muscular support, the mechanical corrections achieved through chiropractic care are harder to maintain between sessions and over time.
A chiropractor treating spinal stenosis will typically prescribe a home exercise program that runs parallel to in-office treatment. These are not generic back exercises — they are selected specifically for the patient’s stenosis level, symptom pattern, and current functional capacity. The exercises are designed to offload pressure from the spine, improve canal space dynamically, and prevent the postural collapse that worsens stenosis symptoms.
The muscles most critical for spinal stenosis management are the deep core stabilisers — the multifidus, transverse abdominis, and pelvic floor — along with the hip flexors and gluteal muscles. These muscle groups work together to maintain spinal alignment under load, reducing the moment-to-moment mechanical stress on compressed spinal segments during daily activity.
Common exercises prescribed for spinal stenosis patients in a chiropractic setting include:
These exercises are generally performed in a flexion-biased position — meaning they favour forward bending rather than backward extension — because spinal flexion opens the posterior canal and reduces nerve compression in stenosis patients. Extension-based exercises like back hyperextensions are typically avoided, especially in the early stages of treatment.
Beyond structured exercise, how a stenosis patient moves throughout the day has a significant impact on symptom levels and treatment outcomes. Chiropractors routinely counsel patients on activity modifications that reduce cumulative spinal load without eliminating movement — because inactivity itself accelerates degeneration.
Walking remains one of the best low-impact activities for spinal stenosis patients, particularly when done with a slight forward lean — such as pushing a walker or shopping cart — which naturally opens the spinal canal. Prolonged standing and walking without rest, however, should be broken into shorter intervals. Sitting for extended periods compresses the lumbar discs and should also be interrupted regularly with brief standing or gentle walking. Simple ergonomic changes — raising a monitor, adjusting a car seat angle, or using a lumbar support cushion — can meaningfully reduce daily spinal strain over time.
The evidence base for chiropractic treatment of spinal stenosis is still developing, but what exists points in a consistent direction. A systematic review published in the Journal of Manipulative and Physiological Therapeutics, which examined all available clinical studies on chiropractic care for lumbar spinal stenosis, concluded that the limited evidence available points toward chiropractic care being potentially beneficial for this patient population. The authors noted that further clinical investigations are necessary, but did not find evidence of harm from appropriately applied chiropractic techniques.
The SPORT study — Spine Patient Outcomes Research Trial — was one of the largest observational studies ever conducted on spinal stenosis treatment outcomes. Among its 368 subjects diagnosed with lumbar spinal stenosis, 33% reported having received chiropractic care as part of their treatment journey. The fact that one in three stenosis patients in a major clinical cohort sought chiropractic care reflects both patient demand and the perceived effectiveness of this approach among those actually living with the condition.
Spinal stenosis is rarely a single-cause problem, and effective management often requires input from more than one provider. Chiropractors treating stenosis frequently work alongside orthopaedic physicians, physical therapists, pain management specialists, and neurologists — particularly in moderate to severe cases where imaging, nerve conduction studies, or epidural steroid injections may be part of the broader treatment plan. This collaborative approach allows chiropractic care to serve as the hands-on, biomechanical component of a larger strategy, addressing the mechanical drivers of symptoms while medical co-managers handle systemic or pharmacological needs.
When it comes to managing spinal stenosis, patients typically face three broad categories of treatment: conservative care (which includes chiropractic), pain management through medication or injections, and surgery. Understanding how these options stack up against each other is critical for making an informed decision.
| Treatment Option | Invasiveness | Recovery Time | Addresses Root Cause | Long-Term Relief |
|---|---|---|---|---|
| Chiropractic Care | Non-invasive | None | Yes — mechanical | Yes, with maintenance |
| Pain Medication | Non-invasive | None | No — symptom masking | Limited |
| Epidural Steroid Injection | Minimally invasive | 1–2 days | No — anti-inflammatory only | Temporary (weeks to months) |
| Physical Therapy alone | Non-invasive | None | Partially | Moderate |
| Laminectomy Surgery | Highly invasive | 3–6 months | Yes — structural | High but with surgical risks |
Medication manages pain but does nothing to address the underlying structural narrowing driving stenosis symptoms. Epidural steroid injections can provide meaningful short-term relief by reducing inflammation around compressed nerve roots, but their effects are temporary and repeated injections carry risks, including tissue thinning and adrenal suppression. Surgery — specifically, a laminectomy, which removes the lamina to decompress the spinal canal — is effective for severe cases but involves significant recovery time, carries surgical risks, and does not guarantee that degenerative changes won’t continue post-operatively. Chiropractic care is the only conservative option that simultaneously addresses spinal alignment, nerve decompression, muscular support, and postural mechanics — without downtime, systemic side effects, or surgical risk.
Surgical intervention for spinal stenosis is sometimes necessary — particularly when neurological deficits are progressive, when bladder or bowel function is compromised, or when conservative care has been exhausted without meaningful improvement. But surgery should be a last resort, not a first response. The clinical reality is that a significant number of patients who pursue conservative chiropractic care first avoid surgery altogether, or at a minimum, enter surgical evaluation with a much clearer picture of what conservative treatment can and cannot resolve for their specific case.
Most spine surgeons themselves recommend a trial of conservative treatment — typically three to six months — before surgical options are seriously considered for non-emergency stenosis cases. Chiropractic care, with its combination of spinal manipulation, decompression therapy, and rehabilitative exercise, is one of the most comprehensive conservative treatments a stenosis patient can undergo. Beginning with chiropractic is not delaying the inevitable — for many patients, it is the solution.
Here are the most common questions patients ask when considering chiropractic care for spinal stenosis, answered directly and without oversimplification.
When performed by a licensed chiropractor who has reviewed imaging and conducted a thorough assessment, chiropractic care for spinal stenosis is considered safe. The systematic review published in the Journal of Manipulative and Physiological Therapeutics found no evidence of harm from appropriately applied chiropractic techniques in spinal stenosis patients.
That said, not every chiropractic technique is appropriate for every stenosis patient. High-velocity lumbar manipulation may be contraindicated in patients with severe canal narrowing, significant instability, or concurrent osteoporosis. A competent chiropractor will modify their approach accordingly — opting for gentler methods like flexion-distraction or spinal decompression therapy when high-velocity manipulation carries unacceptable risk. The key is full disclosure of your diagnosis, imaging findings, and symptom severity before any hands-on treatment begins.
There is no universal answer because stenosis severity, patient age, comorbidities, and response to treatment all vary significantly. However, most chiropractors structure initial spinal stenosis treatment plans around 12 to 20 sessions over four to six weeks, with reassessment at the midpoint to evaluate progress.
Patients with mild to moderate stenosis who respond well early in the treatment plan often transition to a maintenance schedule — less frequent visits designed to preserve the improvements achieved and prevent symptomatic regression. Those with more advanced degeneration may require longer active treatment phases or ongoing co-management with other providers. Expecting a specific number of sessions without a clinical evaluation is unrealistic, but a reputable chiropractor will set clear, measurable goals and timeline expectations from the first appointment.
Severe spinal stenosis — particularly cases involving significant neurological compromise, cauda equina syndrome symptoms, or profound muscle weakness — requires medical evaluation before chiropractic treatment begins. In these situations, chiropractic care may still play a role as part of a co-managed treatment plan, but the chiropractor must work in coordination with a spine specialist. Emergency symptoms such as sudden loss of bladder or bowel control, rapid-onset bilateral leg weakness, or severe progressive neurological deficit require immediate medical attention, not chiropractic care.
Spinal manipulation involves a chiropractor applying a precise, controlled manual force to a specific vertebral joint to restore alignment and improve movement. It is an active, hands-on technique that produces the characteristic audible release sound associated with chiropractic adjustments. The goal is to correct joint mechanics, reduce nerve irritation, and restore proper spinal function at a targeted segment.
Spinal decompression therapy, by contrast, uses a motorised traction table to apply a sustained, rhythmic pulling force along the axis of the spine. It is passive from the patient’s perspective — the machine does the work. The goal is to create negative intradiscal pressure, retract bulging disc material, and physically widen the spinal canal over a series of treatment sessions. For more information on spinal stenosis and its treatment options, you can read about how a chiropractor can help.
Both techniques reduce nerve compression, but through different mechanisms. Manipulation corrects alignment and restores joint mobility; decompression directly reduces structural crowding within the canal. For spinal stenosis, the two are often used together within the same treatment plan — manipulation to restore spinal mechanics, and decompression to address the canal narrowing directly. Flexion-distraction is a bridge between the two: a manual technique that incorporates traction principles without using a motorised table.
Chiropractic care cannot reverse the bony structural changes — the bone spurs, the disc height loss, the thickened ligaments — that are the underlying anatomical cause of spinal stenosis. Those changes are permanent features of spinal degeneration that no conservative treatment can structurally undo without surgery.
What chiropractic care can do — and does effectively for many patients — is manage the functional and symptomatic consequences of those structural changes. By restoring spinal alignment, reducing nerve compression through decompression, strengthening supporting musculature, and improving postural mechanics, chiropractic treatment can keep stenosis symptoms at a level that allows patients to live actively and comfortably, often indefinitely, with appropriate maintenance care.
Think of it less as a cure and more as a management strategy that keeps the condition from running your life. Many patients with confirmed lumbar spinal stenosis on MRI maintain full, active lifestyles through consistent chiropractic care — not because their anatomy changed, but because the functional system around that anatomy was optimised well enough to compensate. For natural, non-surgical spinal stenosis management, exploring what chiropractic care can offer is one of the most informed steps you can take.
About the Author Anthony Kell, D.C., is a Doctor of Chiropractic based in Darlington. He provides expert care at Innovation Central, specialising in spinal health and rehabilitative therapies like Flexion Distraction.
Book Your Slot: 01325 775 240 | [email protected] Learn More: darlingtonchiropracticcare.co.uk
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
You can find more information in our Privacy Policy and .